DOI: 10.31038/IDT.2025611
Introduction
Nocardia species are found in contaminated water and soil [1]. Infections occur due to inhalation of contaminated particles and manifest typically in the lungs, central nervous system, skin, and joints [1,2]. Ocular manifestations include keratitis, scleritis, subretinal abscesses, and endogenous endophthalmitis [1]. Cases of endogenous endophthalmitis have poor visual outcomes and require intravitreal antibiotics [3]. Here we describe a 20-year-old female who presented with pulmonary nocardiosis that disseminated to her brain, lumbar spine and eyes.
Case Report
The patient is an immunosuppressed 20-year-old female with a significant past medical history of moderate developmental delay and systemic lupus erythematosus (SLE) who presented to Akron Children’s Hospital with worsening chest pain following recent pneumonia treatment. A chest CT showed recurrent pleural effusions and pleural fluid culture grew Nocardia cyriacigeorgica. A brain MRI showed numerous enhancing lesions suggestive of disseminated nocardiosis. She was started on oral linezolid and IV ceftriaxone due to a trimethoprim sulfamethoxazole (TMP/SMX) allergy. Ophthalmology was consulted for baseline examination given initiation of long-term oral linezolid therapy.
On initial examination, visual acuity was 20/800 in the right eye and 20/100 in the left. Dilated exam was limited due to patient cooperation but revealed suspected exudative retinal detachment in both eyes. Exam under anesthesia showed subretinal abscess with large serous retinal detachment of the right eye (Figure 1) and a temporal subretinal abscess with serous retinal detachment of the left eye (Figure 2). These findings prompted bilateral intravitreal tap and inject with amikacin. Both vitreous and anterior chamber taps did not yield a positive culture. Weekly intravitreal ceftazidime injections were administered over the next 4 weeks. At discharge, visual acuity was hand motion in the right eye and 20/40 in the left with improvement of serous detachment and abscesses in both eyes. She was discharged on oral TMP/SMX 160mg TID after sensitization and IV ceftriaxone 2g BID with plans to remove the PICC line and switch to oral linezolid 200mg daily in 6 months.
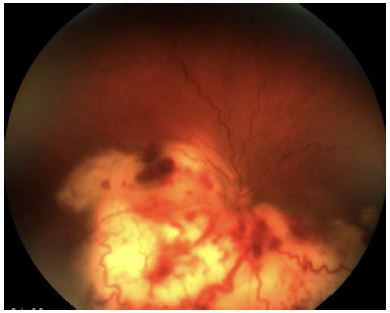
Figure 1: Color fundus photo of right eye with active ocular nocardiosis on initial presentation.
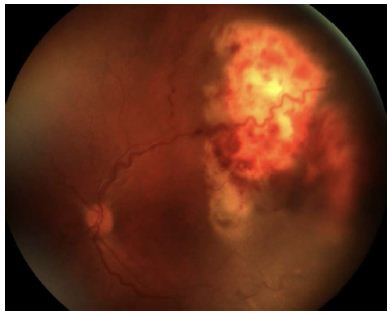
Figure 2: Color fundus photo of left eye with active ocular nocardiosis on initial presentation.
Nine months after discharge, she returned to clinic with increased right eye pain and photophobia raising concern for nocardiosis reactivation. The patient was readmitted and an intravitreal tap and inject with ceftazidime was performed. The sample was improperly processed and did not yield useful data. Topical moxifloxacin, prednisolone QID, and daily atropine were initiated. After five days, her vision was hand motion right eye and 20/60 left eye with almost near resolution of the anterior chamber inflammation. Macular OCT and dilated exam showed stable subretinal fibrosis in both eyes (Figure 3). A PICC line was reinserted, and she was restarted on IV Ceftriaxone 2g BID at the end of her admission.
Due to age and comorbidities, the patient transitioned out of pediatric care. On last chart review, she has since developed choroidal neovascular membrane (CNVM) in the left eye for which she is receiving intravitreal bevacizumab injections.
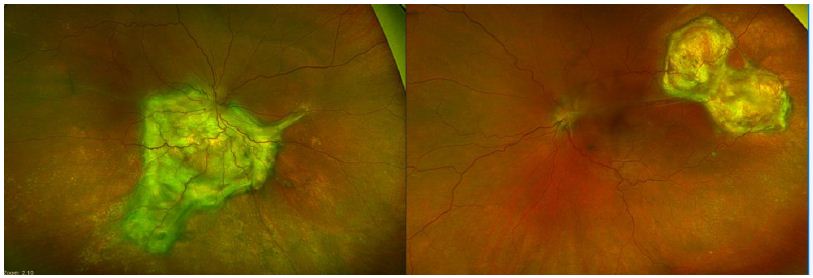
Figure 3: Color fundus photo 9 months after serial intravitreal injections.
Discussion
Nocardia is a gram positive, filamentous, partial acid-fast bacteria that can be found in contaminated water and soil [1]. This patient with SLE on hydroxychloroquine, rituximab and a recent oral steroid taper highlights the increased vulnerability of the immunocompromised population. Primary Nocardia infection is most common in the lungs with the brain being the most likely site of dissemination [1,2]. Ocular involvement is seen in 3-5% of cases often affecting the cornea, sclera, and retina [1-3]. Furthermore, Nocardia is a rare source of endogenous endophthalmitis comprising only 3% of all endophthalmitis cases [2]. Treatment is difficult and visual outcomes are poor.
We present an immunocompromised patient with bilateral subretinal abscesses that were treated successfully with intravitreal antibiotics. Subretinal abscesses can be biopsied to confirm the diagnosis. In our patient, however, the combination of pulmonary, CNS and ocular lesions with a positive pleural fluid culture were sufficient to suggest a Nocardia intraocular infection [4]. Amikacin is a popular antibiotic utilized to treat Nocardia and was used for her first injection [3]. Given sensitivity studies showing susceptibility to ceftazidime and the small risk of associated amikacin macular toxicity, ceftazidime was used for all subsequent intravitreal injections [5]. Our case presented similarly to others in literature in that subretinal fibrotic scarring formed in place of the clearing abscesses [3].
There is no definitive regimen for duration or frequency of intravitreal injections to successfully treat ocular nocardiosis. Our patient developed a suspected reactivation in her right eye after she was switched from IV ceftriaxone to oral linezolid. The reason for the reactivation is unclear given that Nocardia species have near 100% susceptibility to linezolid [6]. Resistance to linezolid is also unlikely given the resolution of the lung and brain lesions. We hypothesize that her reactivation could be due to ending intravitreal injections too early. This case highlights the importance of close multidisciplinary follow up of immunocompromised patients when systemic immunosuppressive medications are adjusted.
References
- DeCroos FC (2004) Optimizing Diagnosis and Management of Nocardia Keratitis, Scleritis, and Endophthalmitis: 11-Year Microbial and Clinical Overview. Ophthalmology 118: 1193-1200.
- Cunha AM, Silva M, Pedrosa AC, Falcão-Reis F, Figueira L (2021) Nocardia Subretinal Abscess: A Rare and Challenging Case Report. Case Reports in Ophthalmological Medicine 2021.
- Hojjatie SL, Salek SS, Pearce WA, Wells JR, Yeh S, et al. (2020) Treatment of presumed Nocardia endophthalmitis and subretinal abscess with serial intravitreal amikacin injections and pars plana vitrectomy. Journal of Ophthalmic Inflammation and Infection 10-14. [crossref]
- Majumder PD, Mukherjee M, Therese L, Gopal L, Biswas J (2018) Diagnostic Challenge with Nocardia Subretinal Abscess: A Case Report from Tuberculosis-Endemic Region. Ocular Immunology and Inflammation 27: 762-765. [crossref]
- Donald D’Amico M, Laure Caspers-Velu M, Jacques Libert M, Shanks E, Schrooyen M, et al. (1985) Comparative Toxicity of Intravitreal Aminoglycoside Antibiotics. American Journal of Ophthalmology 100: 264-275. [crossref]
- Gonzalez A, Fakhar K, Gubernick D, Tuli S (2014) Scleritis Caused by In Vitro Linezolid-Resistant Nocardia asteroides. Case Reports in Ophthalmological Medicine. [crossref]